Even during the current surge, communities with the highest proportion of multi-generational households have seen the largest increase in new COVID-19 cases. To break the chain, we need to test entire households, and not just individuals.
Four Phases
Figure 1 below shows the weekly incidence of newly diagnosed COVID-19 cases in Los Angeles County, running from the week starting March 1 through the week starting November 8, 2020. When we last studied the Los Angeles County epidemic, we saw three distinct phases. Now, we can clearly see four.

During Phase I, which ran through the week of April 4–10, the epidemic spread radially from initial foci of infection located in relatively affluent communities such as the Brentwood and Beverly Crest neighborhoods of Los Angeles and the City of West Hollywood. During Phase II, which ran through the week of July 5-11, COVID-19 incidence rose at slower rate, as coronavirus infections became increasingly concentrated in areas at higher risk of intra-household transmission. During Phase III, which continued until the week of August 30-September 5, COVID-19 incidence gradually declined, while cases continued to accumulate in the same high-risk areas.
Now, we’re in the midst of Phase IV, and cases are again surging. We’ve cut off our graph at the week of November 8-14, as reporting delays prevent us from accurately gauging the full extent of the recent surge. But the incidence of new cases will undoubtedly continue to rise.
Multi-Generational Households
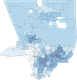
Figure 2 compares two maps of Los Angeles County. Each map is broken down into countywide statistical areas (CSAs), a hybrid geographic classification of independent municipalities such as the City of Beverly Hills, neighborhoods of Los Angeles such as Hollywood, and unincorporated places such as Hacienda Heights.

On the left, the CSAs are color-coded according to the age-adjusted cumulative incidence of COVID-19 per 100,000 population as of November 26, 2020, which we derived from the surveillance dashboard of the Los Angeles County Department of Public Health. On the right, the same CSAs are coded according to the proportion of households that we’ve identified as at risk for multi-generational transmission, which we derived from the 2018 public use microsample of the U.S. Census Bureau’s American Community Survey. As explained in this detailed report, we classified a household as at risk for multi-generational transmission if it had at least four persons, at least one person 18–34 years of age and another person was at least 50 years of age.
The two maps in Figure 2 show just as striking a concordance as when we last performed the comparison. Those communities with the highest prevalence of at-risk households had the highest cumulative incidence of COVID-19 infection.
Within-Household Transmission Has Sustained the Los Angeles County Epidemic
Figure 3 duplicates a pair of graphs that we displayed in our last look at the Los Angeles County epidemic. Both relate the cumulative incidence of COVID-19 infection on the vertical axis to the prevalence of at-risk households across some 300 CSAs in Los Angeles County, as measured on the horizontal axis.
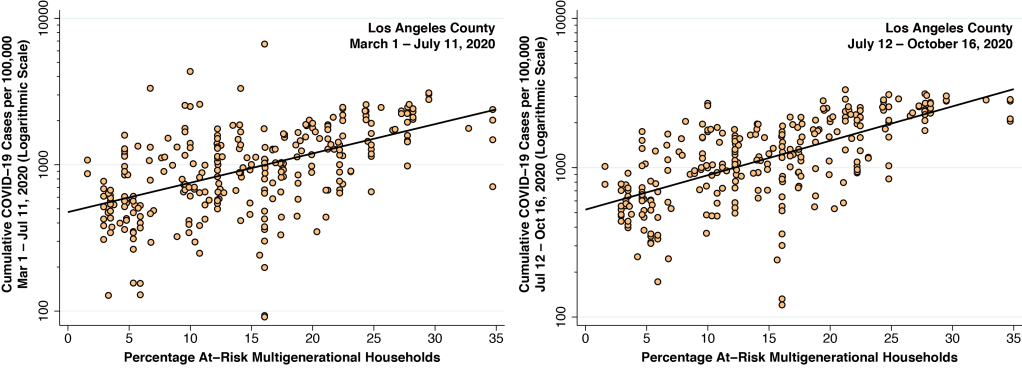
The graph on the left covers cases of COVID-19 diagnosed during Phases I and II, from March 1 through July 11, 2020, when weekly incidence rates were continuing to rise. The graph on the right, by contrast, covers cases diagnosed during Phase III, from July 12 through October 16, when weekly incidence rates turned around and gradually began to fall. Both graphs show a significant positive relationship between the prevalence of at-risk, multi-generational households and the incidence of newly diagnosed coronarvirus infections.
The Catch
Figure 4 repeats the same analysis, covering the cumulative incidence of new cases during Phase IV, from October 17 though November 26. Once again, there is a significant positive relationship across communities between the prevalence of multi-generational households and the incidence of new infections.

The only difference between the plots in Figure 3, which cover Phases I through III of the epidemic, and Figure 4, which covers Phase IV to date, is that the slope of the Phase IV plot is flatter. It remains to be seen whether the slope will stay flatter as backlogged case reports finally make it to the LA County dashboard. If so, it could be an indicator that, while multi-generational household transmission is still a critical vehicle for sustaining the epidemic, the virus has begun to spread outside its established areas of concentration. We need to follow this relationship closely in the coming weeks.
The Negative Feedback Loop
A number of factors, operating in combination, may have triggered the Phase IV surge in Los Angeles County. While it’s nowhere near as cold in Southern California as other parts of the country, nevertheless people are beginning to spend more time indoors. Rising infection rates elsewhere may have led to more importations from outside the county. And then, as we have repeatedly seen in Los Angeles and elsewhere, there is the obvious negative feedback loop. When the epidemic becomes more severe, public officials impose restrictions on social mobility and people take more protective measures. And when the epidemic starts to dissipate, public officials relax restrictions and people drop their guard. That’s why we see the cycles underlying the epidemic curve in Figure 1.
The Multiplier
Whatever the underlying trigger for Phase IV, the high prevalence of multi-generational households in many communities in the Los Angeles area operates as a multiplier. As we noted in our last look, when a younger person, having contracted COVID-19 outside the household, brings his or her infection back home, the impact is magnified by the presence of cohabitants of multiple generations. During our own clinical work, we have recently noted a significant resurgence in the number of infected patients seeking care and advice. Every one of these patients, without exception, has been part of a multi-generational household.
Test Households, Not Just Individuals
A symptomatic patient calls seeking medical advice. She started to feel ill yesterday, but today she has body aches, spiking fevers, and can’t smell her food. She wants to know whether she should get tested. Except as a formality, testing this symptomatic patient is completely uninformative. If the test comes out positive, well, we already knew from the patient’s clinical presentation that she was infected. (A sudden loss of smell in the absence of a completely blocked nose is, by itself, a highly specific test for COVID-19.) And if the test comes out negative, then it was quite likely a false negative and needs repeating.
So, what do we advise the patient? Absolutely everyone in the household has to be tested as soon as possible. Everyone from the toddlers up to the grandparents. The patient may be the first to seek care, but with the high rate of asymptomatic transmission, we need to proactively find out who introduced the infection into the household, who remains susceptible, and who is at risk for the development of severe symptoms in the coming days.